8 Weeks Baby Left Breast Swelling With Lump
This section discusses the symptoms, causes and management of breastfeeding difficulties referred to in Session 5, classified under "Help with difficulties and poor practices. Refer if necessary". Those discussed here include breast conditions and other breastfeeding difficulties, twins, a mother separated from her babe, a child with sickness, abnormality or a status that interferes with suckling, and conditions of the mother. Growth faltering and nonexclusive breastfeeding are discussed in Session v.4; complementary feeding difficulties in Session five.five; and low–nascency-weight infants in Session 6.1.
7.1. Total breasts
Symptoms: Full breasts occur from three–5 days after delivery when the breast milk "comes in". The mother feels uncomfortable and her breasts experience heavy, hot and difficult. Sometimes they are lumpy. The milk flows well, and sometimes drips from the breast.
Cause: This is normal fullness.
Management: The baby needs to be well attached, and to breastfeed often to remove the milk. The fullness decreases afterwards a feed, and after a few days the breasts go more comfortable as milk production adjusts to the baby's needs.
seven.ii. Breast engorgement (1)
Symptoms: The breasts are swollen and oedematous, and the skin looks shiny and diffusely red. Commonly the whole of both breasts are afflicted, and they are painful. The woman may have a fever that usually subsides in 24 hours. The nipples may become stretched tight and flat which makes it difficult for the infant to attach and remove the milk. The milk does not flow well.
Crusade: Failure to remove breast milk, peculiarly in the first few days later on delivery when the milk comes in and fills the chest, and at the same time blood flow to the breasts increases, causing congestion. The common reasons why milk is not removed adequately are delayed initiation of breastfeeding, infrequent feeds, poor attachment and ineffective suckling.
Direction:
-
The mother must remove the breast milk. If the babe can attach well and suckle, and then she should breastfeed equally frequently as the infant is willing. If the infant is non able to attach and suckle effectively, she should express her milk by hand or with a pump a few times until the breasts are softer, so that the baby can adhere ameliorate, and so get him or her to breastfeed oft.
-
She can apply warm compresses to the breast or take a warm shower before expressing, which helps the milk to menstruation. She can utilise cold compresses after feeding or expressing, which helps to reduce the oedema.
-
Engorgement occurs less oftentimes in infant-friendly hospitals which practise the Ten Steps and which help mothers to start breastfeeding soon after delivery.
7.3. Blocked duct
Symptoms: A tender, localised lump in one breast, with redness in the peel over the lump.
Cause: Failure to remove milk from office of the breast, which may be due to infrequent breastfeeds, poor attachment, tight wear or trauma to the breast. Sometimes the duct to one function of the breast is blocked by thickened milk.
Management: Amend removal of milk and correct the underlying crusade.
-
The mother should feed from the affected breast frequently and gently massage the chest over the lump while her baby is suckling.
-
Some mothers discover it helpful to apply warm compresses, and to vary the position of the baby (across her body or under her arm).
-
Sometimes after gentle massage over the lump, a string of the thickened milk comes out through the nipple, followed by a stream of milk, and rapid relief of the blocked duct.
seven.4. Mastitis (2)
Symptoms: There is a hard swelling in the breast, with redness of the overlying skin and severe pain. Ordinarily just a role of one breast is affected, which is dissimilar from engorgement, when the whole of both breasts are afflicted. The woman has fever and feels ill. Mastitis is commonest in the first 2–iii weeks after delivery but can occur at whatsoever time.
Causes: An of import cause is long gaps between feeds, for example when the mother is decorated or resumes employment outside the home, or when the baby starts sleeping through the nighttime. Other causes include poor attachment, with incomplete removal of milk; unrelieved engorgement; frequent pressure on i part of the chest from fingers or tight clothing; and trauma. Mastitis is ordinarily caused in the first place by milk staying in the breast, or milk stasis, which results in non-infective inflammation. Infection may supervene if the stasis persists, or if the woman as well has a nipple scissure that becomes infected. The condition may then become infective mastitis.
Management: Improve the removal of milk and attempt to correct any specific crusade that is identified.
-
Advise the mother to rest, to breastfeed the baby oftentimes and to avoid leaving long gaps between feeds. If she is employed, she should take sick leave to remainder in bed and feed the baby. She should not end breastfeeding.
-
She may discover information technology helpful to apply warm compresses, to start breastfeeding the baby with the unaffected chest, to stimulate the oxytocin reflex and milk flow, and to vary the position of the babe.
-
She may take analgesics (if bachelor, ibuprofen, which also reduces the inflammation of the breast; or paracetamol).
-
If symptoms are astringent, if there is an infected nipple fissure or if no improvement is seen after 24 hours of improved milk removal, the handling should then include penicillinase-resistant antibiotics (e.thousand., flucloxacillin). However antibiotics will not be effective without improved removal of milk.
7.five. Chest abscess (ii)
Symptoms: A painful swelling in the chest, which feels full of fluid. There may exist discoloration of the peel at the point of the swelling.
Cause: Ordinarily secondary to mastitis that has non been effectively managed.
Management: An abscess needs to be drained and treated with penicillinase-resistant antibiotics. When possible drainage should exist either by catheter through a pocket-sized incision, or by needle aspiration (which may need to be repeated). Placement of a catheter or needle should be guided past ultrasound. A large surgical incision may impairment the areola and milk ducts and interfere with subsequent breastfeeding, and should exist avoided. The mother may go along to feed from the affected breast. Withal, if suckling is too painful or if the female parent is unwilling, she can exist shown how to express her milk, and brash to let her infant offset to feed from the breast again equally soon as the pain is less, normally in 2–iii days. She can go along to feed from the other breast. Feeding from an infected breast does not affect the infant (unless the mother is HIV-positive, come across Session 7.7).
Sometimes milk drains from the incision if lactation continues. This dries up afterwards a time and is not a reason to stop breastfeeding.
7.6. Sore or fissured nipple
Symptoms: The mother has astringent nipple hurting when the babe is suckling. There may be a visible scissure beyond the tip of the nipple or effectually the base of operations. The nipple may await squashed from side-to-side at the stop of a feed, with a white pressure level line across the tip.
Cause: The main cause of sore and fissured nipples is poor attachment. This may exist due to the infant pulling the nipple in and out as he or she suckles, and rubbing the peel against his or her mouth; or it may be due to the potent pressure on the nipple resulting from incorrect suckling.
Management: The mother should be helped to improve her baby'due south position and attachment. Often, as before long every bit the infant is well fastened, the pain is less. The baby can continue breastfeeding commonly. At that place is no need to rest the chest – the nipple will heal quickly when it is no longer being damaged.
7.7. Mastitis, abscess and nipple scissure in an HIV-infected adult female (2)
If a woman is HIV-infected, mastitis, breast abscess and nipple fissure (particularly if the nipple is haemorrhage or oozing pus) may increase the risk of HIV manual to the infant. The recommendation to increase the frequency and duration of feeds is non advisable for a mother who is HIV-positive.
Management for a woman who is HIV-positive:
-
She should avert breastfeeding on the affected side while the condition persists.
-
She should remove the milk from the affected breast by expression, to help the chest to recover and to maintain the flow of milk. She should exist helped to make sure that she can limited her milk effectively.
-
If but one chest is affected, the baby can continue to feed on the unaffected breast, and can feed more than often from that side to increase production and ensure an acceptable intake.
-
Requite antibiotics for ten–xiv days, rest and analgesics as required, and incision if there is an abscess, equally for an HIV-negative woman.
-
She can resume breastfeeding from the afflicted breast when the status subsides.
-
Some mothers make up one's mind to stop breastfeeding at this fourth dimension if they are able to give replacement feeds safely. They should continue to express enough milk to permit the breasts to recover, until milk product ceases.
-
If both breasts are affected, she will non be able to feed the babe from either side, and will need to consider other feeding options as a permanent solution. She may make up one's mind to heat-treat her own milk and give that, or to give formula. She should feed the baby by loving cup.
7.8. Candida infection (thrush) in mother and baby (3)
Symptoms:
In the mother:
-
Sore nipples with pain continuing between feeds, pain like sharp needles going deep into the breast, which is not relieved by improved zipper.
-
There may exist a red or flaky rash on the areola, with itching and depigmentation.
In the babe:
-
White spots inside the cheeks or over the tongue, which await like milk curds, but they cannot be removed easily.
-
Some babies feed commonly, some feed for a short time and so pull away, some refuse to feed birthday, and some are distressed when they try to attach and feed, suggesting that their mouth is sore.
-
There may be a red rash over the nappy area ("diaper dermatitis").
Cause: This is an infection with the fungus Candida albicans, which oft follows the use of antibiotics in the baby or in the mother to treat mastitis or other infections.
Management: Treatment is with gentian violet or nystatin. If the mother has symptoms, both mother and babe should be treated. If only the baby has symptoms, it is not necessary to treat the mother.
Gentian Violet pigment:
Utilize 0.25% solution to babe'southward mouth daily for 5 days, or until 3 days after lesions heal.
Apply 0.5% solution to mother's nipples daily for 5 days.
Nystatin:
Nystatin suspension 100,000 IU/ml; utilise 1 ml by dropper to kid'due south mouth 4 times daily later on breastfeeds for 7 days, or as long as the mother is beingness treated.
Nystatin cream 100,000 IU/ml; employ to nipples 4 times daily afterward breastfeeds. Continue to apply for 7 days afterwards lesions take healed.
vii.ix. Inverted, flat, large and long nipples (iii)
Signs to look for: Nipples naturally occur in a broad variety of shapes that normally practise not impact a mother's ability to breastfeed successfully. All the same, some nipples look flat, large or long, and the baby has difficulty attaching to them. Nigh flat nipples are protractile –if the mother pulls them out with her fingers, they stretch, in the same way that they take to stretch in the baby'south mouth. A baby should have no difficulty suckling from a protractile nipple. Sometimes an inverted nipple is non-protractile and does non stretch out when pulled; instead, the tip goes in. This makes it more hard for the babe to adhere. Protractility often improves during pregnancy and in the first calendar week or and so after a baby is born. A big or long nipple may make information technology hard for a baby to take plenty breast tissue into his or her oral fissure. Sometimes the base of the nipple is visible even though the baby has a widely-open oral fissure.
Cause: Different nipple shapes are a natural physical characteristic of the breast. An inverted nipple is held past tight connective tissue that may slacken afterwards a babe suckles from it for a fourth dimension.
Management: The same principles utilise for the management of apartment, inverted, large or long nipples.
-
Antenatal treatment is not helpful. If a pregnant woman is worried about the shape of her nipples, explain that babies can often suckle without difficulty from nipples of unusual shapes, and that skilled aid later on delivery is the most important thing.
-
Equally soon every bit possible after delivery, the mother should exist helped to position and effort to attach her baby. Sometimes it helps if the mother takes a different position, such as leaning over the baby, then that the chest and nipple driblet towards the babe's mouth.
-
The mother should give the baby enough of skin-to-pare contact near the breast, and permit the infant try to find his or her ain way of taking the breast, which many do.
-
If a infant cannot attach in the starting time week or two, the female parent can express her chest milk and feed it by cup.
-
The female parent should go on putting the babe to the breast in different positions, and allowing him or her to try. She can express milk into the baby's oral cavity, and touch the lips to stimulate the rooting reflex and encourage the baby to open up his or her oral cavity wider.
-
As a infant grows, the oral cavity soon becomes larger, and he or she tin can attach more easily.
-
Feeding bottles or dummies, which do non encourage a baby to open the rima oris wide, should exist avoided.
-
For apartment or inverted nipples, a mother can use a 20 ml syringe, with the adaptor finish cut off and the plunger put in backwards to stretch out the nipple just earlier a feed (meet Figure 20).
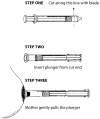
Effigy 20
Preparing and using a syringe for treatment of inverted nipples.
seven.x. Perceived insufficiency and low breast-milk production
Symptoms: The commonest difficulty that mothers draw is a feeling that they do non have enough milk. In many cases, the infant is in fact getting all the milk that he or she needs, and the trouble is the female parent's perception that the milk supply is insufficient.
In some cases, a baby does have a depression intake of breast milk, insufficient for his or her needs. Occasionally, this is because the mother has a physiological or pathological low breast-milk production (iv). Normally, still, the reason for a low intake is a faulty technique or pattern of feeding. If the breastfeeding technique or pattern improves, the baby's intake increases. When a infant takes only function of the milk from the breast, production decreases, but it increases again when the baby takes more than.
Symptoms which make a mother call up that her breast milk is insufficient include:
-
the baby crying a lot, and seeming not to be satisfied with feeds;
-
the baby wanting to feed very often or for a long fourth dimension at each feed;
-
the breasts feeling soft;
-
not beingness able to express her milk.
These symptoms tin occur for other reasons, and they do not necessarily show that a babe's intake is depression.
If a mother is worried about her milk supply, it is necessary to decide if the baby is taking plenty milk or not.
If the baby has a low milk intake, then it is necessary to find out if it is due to breastfeeding technique, or low breast-milk production.
If the baby'southward intake is acceptable, so information technology is necessary to decide the reasons for the signs that are worrying the mother.
LOW Chest-MILK INTAKE
Signs: In that location are 2 reliable signs that a infant is non getting enough milk:
-
poor weight gain.
-
low urine output.
Passing meconium (mucilaginous black stools) four days after delivery is also a sign of the infant not getting enough milk.
Poor weight gain
Babies' weight proceeds is variable, and each child follows his or her own pattern. You cannot tell from a single weighing if a baby is growing satisfactorily – it is necessary to weigh several times over a few days at least (run into Annex three for tables showing the range of weights for babies of different birth weights).
Presently after nascence a baby may lose weight for a few days. Most recover their birth weight past the end of the first calendar week, if they are healthy and feeding well. All babies should recover their birth weight by 2 weeks of historic period. A baby who is below his or her birth weight at the finish of the 2d week needs to be assessed.
From 2 weeks, babies who are breastfed may gain from most 500 chiliad to ane kg or more each month. All these weight gains are normal. The babe should exist checked for affliction or congenital abnormality and urine output. The technique and blueprint of breastfeeding, and the mother-babe interaction should also be assessed, to decide the crusade of poor weight gain, as explained beneath.
Low Urine Output
An exclusively breastfed baby who is taking enough milk unremarkably passes dilute urine vi-8 times or more in 24 hours. If a babe is passing urine less than 6 times a day, especially if the urine is dark yellow and potent smelling, then he or she is not getting enough fluid. This is a useful way to detect out quickly if a baby is probably taking enough milk or non. However, information technology is non useful if the baby is having other drinks in add-on to breast milk.
Causes: The reasons for a depression chest-milk intake are summarised in Table 9, and classified equally breastfeeding factors; psychological factors with female parent; mother's physical condition; and baby's condition (illness or aberration).
TABLE 9
Reasons why a baby may not get enough chest milk.
Breastfeeding factors
A low breast-milk intake may be due to:
-
delayed initiation of breastfeeding, so that milk production does not adjust in the early days to match the babe's needs;
-
poor attachment, so that the infant does not take the milk from the breast efficiently;
-
infrequent feeds, feeds at stock-still times or no night feeds, and then that the baby simply does non suckle enough; breastfeeding less than 8 times in 24 hours in the get-go viii weeks, or less than v–6 times in 24 hours after eight weeks;
-
short feeds, if a mother is very hurried, or if she takes the baby off the breast during a break earlier he or she has finished, or if the infant stops speedily considering he is wrapped up and too hot, and then he or she may not take every bit much milk as needed, especially the fatty-rich hind milk;
-
using bottles or pacifiers which replace suckling at the breast, so the baby suckles less. Babies who utilize pacifiers tend to breastfeed for a shorter period. Pacifiers may be a marker or a crusade of breastfeeding failure (5). They may interfere with attachment, and so the infant suckles less effectively;
-
giving other foods or drinks causes the baby to suckle less at the breast and take less milk, and also stimulates the chest less, then less milk is produced.
Psychological factors of the female parent
A female parent may exist depressed, lacking in confidence, worried, or stressed; or she may pass up the baby or dislike the idea of breastfeeding. These factors do not directly bear on her milk production, but can interfere with the manner in which she responds to her babe, and then that she breastfeeds less. This can result in the infant taking less milk, and failing to stimulate milk production.
Mother'south physical status
A few mothers have low milk product for a pathological reason including endocrine bug (pituitary failure after astringent bleeding, retained piece of placenta) or poor breast evolution. A few mothers have a physiological low breast-milk production, for no apparent reason, and product does not increase when the breastfeeding technique and pattern improve.
Other factors that tin can reduce milk product temporarily include hormone-containing contraceptive pills, pregnancy, severe malnutrition, smoking and booze consumption.
Baby'southward condition
A baby may fail to gain weight, or may fail to breastfeed well and stimulate milk production because of illness, prematurity or congenital abnormality, such as a palate defect, centre status or kidney aberration. It is always of import to consider these factors and to examine a infant carefully before terminal that a mother has low breast-milk product.
Decision
The common reasons for a baby not getting plenty breast milk are due to poor technique or mismanagement of breastfeeding, which can be overcome. Only a few mothers have long-term difficulty with milk product.
PERCEIVED INSUFFICIENCY
Signs: If a babe is gaining weight co-ordinate to the expected growth velocity, and is passing dilute urine half dozen or more than times in 24 hours, then his or her milk intake is acceptable. If the mother thinks that she does not have enough milk, then it is perceived insufficiency.
Causes: Poor attachment is likely to be the cause if a infant:
-
wants to feed very often (more often than 2 hourly all the time, with no long intervals betwixt feeds);
-
suckles for a long fourth dimension at each feed (more than one one-half hour, unless newborn or low nascence weight);
-
is generally unsettled.
Management of perceived insufficiency and low breast milk production: A health worker may use counselling skills to listen and learn, to take a feeding history and to sympathize the difficulty, particularly if there may be psychological factors affecting breastfeeding. A breastfeed should be observed, checking the baby's attachment. The female parent's physical status and the baby'southward condition and weight should also be noted. A health worker should decide if the difficulty is due to depression milk intake, or perceived insufficiency.
If the difficulty is low milk intake, a health worker should:
-
decide the reason for the depression milk intake;
-
treat or refer the baby, if there is any illness or abnormality;
-
assistance the mother with any of the less common causes, for example if she is using oestrogen-containing contraceptive pills. Referral may exist necessary;
-
hash out how the mother can improve her breastfeeding technique and pattern and improve the baby'due south attachment;
-
use counselling skills to assistance her with whatever psychological factors, and to build her conviction in her milk supply.
If the difficulty is perceived insufficiency, the health worker should:
-
determine the reason;
-
explicate the difficulty, and what might assist;
-
discuss how the mother can better her breastfeeding technique and pattern, and help her to improve the baby'southward zipper;
-
if the baby has reflux, suggest that she holds him or her in a more upright position;
-
use counselling skills to aid the mother with any psychological factors, and to build her confidence in her milk supply.
7.11. Crying baby
Signs or symptoms: The baby cries excessively, and is hard to comfort. The blueprint of crying may suggest the crusade.
Cause:
-
Pain or illness. This may be the instance when a baby of a sudden cries more than than before.
-
Hunger due to sudden faster growth, common at ages 2 weeks, 6 weeks and three months (sometimes called a "growth spurt"). If the baby feeds more oft for a few days, the breast milk supply increases and the problem resolves.
-
Sensitivity to substances from the mother'southward food. This may be any nutrient, but is unremarkably milk, soy, egg or peanuts. Caffeine in coffee, tea and colas, and substances from cigarette smoke can as well upset a babe. If the female parent avoids the nutrient or potable that may exist causing the trouble, the infant cries less.
-
Gastro-oesophageal reflux. The baby cries afterward feeds, often on lying down, and may vomit a large amount of the feed, more than the slight regurgitation that is very mutual. The opening betwixt the oesophagus and the stomach (cardiac orifice) is weak, allowing milk to flow back into the oesophagus, which can cause hurting.
-
Colic. Oft crying occurs at certain times of day, typically the evening. The babe may pull up his legs equally if in pain. He or she wants to feed but is difficult to comfort. The cause is non clear. Babies with colic ordinarily grow well, and the crying decreases later 3–4 months. Carrying the baby more, using a gentle rocking move, and pressure on the belly with the hands, or against the shoulder, may help.
-
High-needs babies. Some babies cry more than others, and they need to be carried and held more. This problem is less common in communities where mothers carry their babies with them, and keep them in the same bed.
Management:
-
If a specific cause, such as hurting or illness, can be identified, information technology should exist treated.
-
The female parent can try a change in her diet, such as stopping drinking milk or coffee for a calendar week, to encounter if there is an improvement.
-
Holding the baby upright may help reflux, or medication may be suggested.
-
For colic or a high-needs baby, the female parent can carry and stone the infant with gentle pressure on the abdomen. She may need reassurance that the crying volition lessen equally the baby grows.
7.12. Oversupply of breast milk
Symptoms:
-
The babe cries as if he or she has colic and wants to feed ofttimes.
-
The baby may have frequent loose stools, which may be green.
-
He or she may abound well, or may take poor weight gain, suggesting low milk production.
-
The mother may have a forceful oxytocin reflex, so that her milk flows fast. This can brand the baby choke and pull abroad from the breast during feeds.
Crusade:
-
The baby may be poorly attached, and suckling a lot but non removing the milk efficiently. Abiding suckling may stimulate the chest to produce a lot of milk.
-
The female parent may have her baby off the first breast before he or she has finished to put him on the 2nd breast. The baby may get mostly low-fat fore milk, and suckle more to get more than energy, and so stimulate the breasts to brand more milk.
-
Large amounts of foremilk overload the babe with lactose, causing loose stools and colicky behaviour.
Management:
-
The mother should be helped to improve her babe's attachment.
-
The female parent should offer but one breast at each feed, until the baby finishes by him- or herself. The infant will go more fat-rich hindmilk. She should offer the other chest at the next feed.
-
If a forceful oxytocin reflex continues, she tin can lie on her back to breastfeed, or hold the breast with her fingers closer to the areola during feeds.
7.13. Refusal to breastfeed
Symptoms: The baby refuses to breastfeed, and may cry, curvation his or her back, and plow away when put to the breast. The mother may feel rejected and frustrated, and exist in neat distress.
Causes: At that place may exist a concrete problem such every bit:
-
illness, an infection, or a sore mouth, for example thrush (see Session 7.8);
-
pain, for example bruising later on a traumatic delivery or gastro-oesophageal reflux;
-
sedation, if the female parent received analgesics during labour.
The baby may have difficulty or frustration with breastfeeding because of:
-
sucking on a bottle or pacifier;
-
difficulty attaching to the breast;
-
pressure applied to his or her caput by someone helping with positioning;
-
the female parent shaking her breast when trying to adhere him or her.
The baby may be upset past a change in the environment including:
-
a changed routine, the mother resuming employment or moving house;
-
a different carer, or as well many carers;
-
a change in the mother's smell – for example, if she uses a different soap or perfume.
Direction: If a cause is identified, it should exist treated or removed, if possible.
The mother could consider how she can reduce the fourth dimension she spends abroad from the baby, or avert other changes that may be upsetting. She tin can exist helped to improve her breastfeeding technique, and how to avoid the use of bottles and pacifiers. She can as well be helped to:
-
proceed her baby close, with plenty of peel-to-pare contact, and no other carers for a time;
-
offer her breast whenever the infant shows signs of interest in suckling;
-
express milk into the babe's mouth;
-
avoid shaking her breast or pressing the baby's head to forcefulness him or her to the breast;
-
feed the baby by cup, if possible with her own breast milk, until he or she is willing to take the breast again.
7.14. Twins
Direction
Twins who are low birth weight need to exist managed accordingly (come across Session six.1).
For larger twins, management should be as for singletons, with early on contact, aid to achieve proficient attachment at the breast, and exclusive on-demand feeding from nativity, or from as presently every bit the mother is able to respond. Early on constructive suckling tin ensure an adequate milk supply for both infants.
Mothers may need aid to discover the best way to agree two babies to suckle, either at the same time, or one at a time. They may similar to requite each baby its own breast, or to vary the side. Holding one or both babies in the underarm position for feeding, and support for the babies with pillows or folded clothes is often helpful. Building the female parent's conviction that she tin make enough milk for 2, and encouraging relatives to help with other household duties, may assistance her to avoid trying to feed the babies artificially.
seven.15. Caesarean section
Management
Initiating breastfeeding
Mothers and babies delivered by caesarean department can breastfeed normally, unless there is some other complication, such as illness or abnormality.
If the mother has had spinal or epidural anaesthesia, the infant should be delivered onto her chest, and she can start skin-to-peel contact and initiate breastfeeding during the first hour in a similar way to that after vaginal delivery.
If she has had a general anaesthetic, she should outset skin-to-skin contact and initiate breastfeeding every bit soon as she is able to respond, usually about 4 hours after delivery. A baby who is full term and in good status tin look for the first feed until the mother responds. Babies who are at chance of hypoglycaemia may need an alternative feed until they can start breastfeeding (come across Session 6.i). Any other feeds should exist given by cup then that they do not interfere with subsequently establishment of breastfeeding.
Later feeds
Afterward caesarian department, a female parent should keep to feed her baby on demand, but she will need aid for a few days to hold the baby, to learn how to breastfeed lying downwardly, and to turn over and to position herself comfortably for feeds (encounter Session 2.11). Infirmary staff and family unit members can all aid her in this way.
Nearly mothers can breastfeed normally afterward a caesarean commitment if they are given appropriate help. Difficulties in the past take often been because mothers did non receive enough assist to constitute breastfeeding in the post-operative flow, and because babies were given other feeds meanwhile.
If a babe is too ill or too small to fed from the chest soon afterward delivery, the mother should exist helped to limited her milk to establish the supply, starting within 6 hours of commitment or equally soon equally possible, in the same style as after a vaginal commitment (see Session 4.5). The EBM tin be frozen for use when the baby is able to accept oral feeds.
If the mother is also sick to breastfeed, the baby should be given artificial milk or banked breast milk by loving cup until the female parent is able to offset breastfeeding.
7.16. Female parent separated from her baby
Short-TERM SEPARATION SUCH Equally EMPLOYMENT OUTSIDE THE HOME
The commonest reason for a mother being separated from her baby for part of the day is because she is employed outside the home, for example when maternity leave is not adequate to enable her to continue breastfeeding exclusively for 6 months.
Management
Options should exist discussed with the mother. She should be encouraged to breastfeed the baby as much equally possible when she is at home, and to consider expressing her milk to leave for someone else to give to her infant.
Expressing her milk for the baby
A trained health worker should teach her how to express and store her breast milk (encounter Session 4.5), how to feed her baby by loving cup (Session iv.vi), and why information technology is best to avoid using a feeding bottle.
How to maintain her milk supply
She should:
-
breastfeed her baby whenever she is at home, such as at night and weekends;
-
slumber with her babe, then that she tin breastfeed at dark and early in the morning;
-
limited milk in the morn before she leaves for work;
-
express her milk while she is at work to proceed up the supply. She tin air-condition the milk if this is possible, or proceed it for up to 8 hours at room temperature and bring it home. If this is non possible, she may have to discard it. She needs to understand that the milk is not lost – her breasts volition make more. If a mother does not express when at work, her milk production volition subtract.
TEMPORARY SEPARATION FOR OTHER REASONS
A mother and her baby may be separated and unable to breastfeed if either of them is ill and admitted to infirmary, or if the baby is LBW or has bug at nascency and is in the Special Intendance Baby Unit of measurement (encounter Session half-dozen.ane).
Direction
While separated, encourage the female parent to express her milk as often as the baby would feed, in lodge to establish or proceed upwards the supply. If facilities are available, she tin can store her milk by freezing it (see Session 4.five). Help the baby to outset breastfeeding equally soon as he or she is able and tin can be with the mother again.
7.17. Illness, jaundice and aberration of the child
ILLNESS
Symptoms related to feeding
-
The infant may want to breastfeed more oft than before.
-
Local symptoms such as a blocked olfactory organ, or oral thrush tin interfere with suckling. The baby may suckle for only a brusque fourth dimension and not take enough milk.
-
The infant may be too weak to suckle adequately, or may exist unable to suckle at all.
-
During surgery an baby may non exist able to receive any oral or enteral feeds.
Management: Infants and immature children who are sick should continue to breastfeed as much as possible, while they receive other treatment. Breast milk is the ideal food during disease, especially for infants less than 6 months old, and helps them to recover.
Babies nether six months of historic period
If a baby is in hospital, the female parent should be immune to stay with him or her, and to have unrestricted admission so that she can respond to and feed the babe equally needed.
If a baby has a blocked nose
The female parent tin be taught how to use drops of salted water or breast milk, and clear the infant'due south nose by making a wick with a twist of tissue. She can give shorter more frequent breastfeeds, allowing the baby time to pause and breathe through the mouth until the nose clears.
If a baby has a sore mouth considering of thrush (Candida)
The female parent'due south nipple and the baby's oral fissure should both be treated with gentian violet or nystatin (see Session 7.eight).
If a baby is not able to breastfeed adequately, but can take oral or enteral feeds
The mother can express her milk (see Session iv.5). She should limited every bit frequently every bit the infant would feed, that is eight times in 24 hours, to keep upwardly her milk supply. The female parent tin feed her EBM to the babe past loving cup or nasogastric tube or syringe. She should exist encouraged to allow the baby suckle whenever he or she wants to.
If a baby is not able to take any oral or enteral feeds
The mother should exist encouraged to continue expressing to keep up her milk supply. Her expressed milk tin be stored safely and given to the baby as soon as he or she starts enteral feeds. She can resume breastfeeding every bit the baby recovers. She may exist able to freeze unused milk for later use. If the hospital has milk-banking facilities, the milk may be used for some other child.
If breast-milk production decreases during an illness
A subtract in production is especially likely if a mother has breastfeeding difficulties or if she has given inappropriate supplements. Feeding difficulties and supplements may have contributed to the infant'southward illness, and are an important crusade of malnutrition. The female parent needs aid to increase her milk supply once again. The female parent should be encouraged to relactate, and to feed her babe using supplementary suckling to stimulate breast-milk production (see Session half dozen.4). With appropriate skilled support, many mothers tin resume sectional breastfeeding inside 1–2 weeks.
Infants and young children over 6 months of age
A young child may prefer breastfeeding to complementary foods while he or she is sick, and breastfeed more than before. Milk production may increase, so that the mother notices increased fullness of her breasts. She should exist encouraged to stay with her child in hospital and to breastfeed on demand.
The mother or caregiver should continue to offer complementary foods, which may need to exist given more often, in smaller quantities and of a softer consistency than when the kid is well. Offering actress food during recovery every bit the child's ambition increases.
JAUNDICE
Symptoms
Early jaundice appears betwixt two and seven days of life. It is usually physiological, and clears after a few days. Jaundice can make a baby sleepy so that he or she suckles less. Early on initiation of breastfeeding and frequent breastfeeding reduce the severity of early on jaundice.
Prolonged jaundice starts later the seventh day of life and continues for some weeks. It is ordinarily due to hormones or other substances in the mother's milk, so it is sometimes called "breast-milk jaundice" which is harmless and clears past itself. If the jaundice is due to a more serious status there are commonly other signs, such equally pale stools, dark urine, or enlarged liver and spleen.
Management
Early on jaundice
Water and glucose water do not aid, and may make a infant suckle less at the breast. Taking more chest milk helps jaundice to articulate more quickly, and so the female parent should be encouraged to breastfeed equally often as her baby is willing. She can also express her milk after feeds and requite some extra by cup or tube. If she is feeding her baby on expressed breast milk, she should give xx% actress. If jaundice is severe, phototherapy (light treatment) may be needed.
Prolonged jaundice
The babe should exist referred for clinical cess, to exclude a serious status. The mother should go along breastfeeding until the baby has been fully assessed.
ABNORMALITIES
Symptoms
Cleft lip and/or palate: attachment and suckling may be difficult because of the anatomical gap. If simply the lip is affected, the breast covers the cleft, and the baby may exist able to suckle finer. Sometimes a baby with a scissure palate can suckle quite well, if there is plenty palate for the tongue to press the nipple against.
Natural language-tie: the strip of tissue underneath the tongue, called the frenulum, is too short and holds the tongue downward. This can make zipper difficult, which may cause sore nipples. The infant may not suckle effectively and may take a low intake of breast milk.
Muscular weakness: babies with Downwardly syndrome or cerebral palsy have difficulty attaching to the chest and suckling because of the weakness.
Built heart or kidney problems: a babe fails to abound, but in that location is no apparent difficulty with breastfeeding or breast-milk supply. These abnormalities are non obvious, and crave careful examination of the baby.
Management
Cleft lip and/or palate
The baby should exist referred for surgery, which unremarkably takes place in one or more stages after some months. It is of import for the baby to grow and to be well nourished before undergoing surgery.
The mother can be helped to hold the babe in an upright sitting position at the chest with the baby's legs on either side of the female parent'south thigh. This makes swallowing easier and may aid the infant to breastfeed, fully or partially. She can express her milk and feed information technology to the baby past cup or spoon until surgical assist is bachelor, or an orthopaedic device is provided to facilitate breastfeeding.
The family unit may need a swell bargain of support and help to have the baby, to persist with feeding, and to believe that the baby volition await almost normal and volition be able to atomic number 82 a normal life if he or she has surgery.
Natural language-tie
If tongue-necktie is causing problems with feeding, the baby will need referring for cutting of the frenulum.
This is constructive and can at present be washed simply and safely (6).
Muscular weakness
The mother should be shown how to help the baby to attach to the breast past using the dancer hand position (Figure 21). She supports the baby'southward mentum and head to keep the oral cavity close on to the breast. These babies may feed slowly, and it may be necessary for the mother to limited her milk and give some feeds by loving cup or tube. The female parent will demand actress support and counselling to bond with her baby, to experience that she is doing the best for him or her, and to persist.

Heart, kidney or other abnormalities
Consider these possibilities in a baby who fails to grow despite good breastfeeding practices. Examine the baby carefully, and refer for further cess.
References
- 1.
-
WHO. Show for the Ten Steps to successful breastfeeding. Geneva: World Wellness Organization; 1998.
- 2.
-
WHO. Mastitis: causes and management. Geneva: Globe Health Organization; 2000. (WHO/FCH/CAH/00.13)
- iii.
-
Mohrbacher N, Stock J. The breastfeeding answer book. 3rd revised ed. Schaumburg, Illinois, USA: La Leche League International; 2003. [4 November 2008]. http://world wide web
.lalecheleague.org. - 4.
-
Woolridge MW. Breastfeeding: physiology into do. In: Davies DP, editor. Nutrition in child health. London: Royal College of Physicians of London; 2003.
- v.
-
Kramer MS, et al. Pacifier use, early weaning, and cry/fuss beliefs: a randomized controlled trial. Journal of the American Medical Association. 2001;286:322–326. [PubMed: 11466098]
- 6.
-
Hogan M, Westcott C, Griffiths One thousand. Randomized control trial of partitioning of tongue-tie in infants with feeding problems. Journal of Paediatrics and Child Health. 2005;41:246–250. [PubMed: 15953322]
henryyousuponchis.blogspot.com
Source: https://www.ncbi.nlm.nih.gov/books/NBK148955/
Postar um comentário for "8 Weeks Baby Left Breast Swelling With Lump"